
Dr. Kristin Tully and Ty Hagler at Innovation Carolina in the Research Triangle Park
To address modern patient health and safety needs, there is a clear and urgent need for innovation in infant hospital bassinet design. Existing infant bassinets consist of an acrylic tub on a wheeled cart and were designed for nurses caring for multiple infants in a common nursery, rather than for one-on-one care in the mother’s room. Individual mother-infant rooming-in is the current standard of healthcare; however, existing bassinets remain in use and they increase risk for women and their infants. By requiring mothers to either substantially twist their bodies to access their infants or get up out of bed to reach them, existing bassinet designs expose new mothers to unnecessary pain or even to post-cesarean injury (Tully & Ball, 2014).
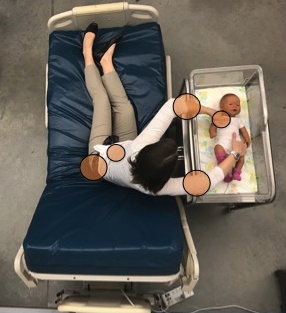
Unmet Needs – Pain Points Contribute to Risk
Impeded maternal access to babies also undermines breastfeeding, which requires recognition of infant cues and the ability to put infants to the breast frequently (Tully, Ball, & Ward-Platt, 2015). In the absence of family members to provide assistance, mothers must call upon healthcare providers for non-medical needs such as infant diaper changes. This can result in delay of medical care for others and maternal frustration at being unable to attend to infants. As importantly, this places an additional and unnecessary burden on healthcare staff (Taylor, Tully & Ball, 2016).
Further, existing bassinets directly expose infants to physical risk. High bassinet walls on all four sides of bassinets create an access barrier for new mothers. This iatrogenic obstacle contributes to the newborns being in the maternity bed or on chairs while the adult is asleep, instead of placed back into the bassinet. This coping strategy while rooming-in on the postnatal unit leads to infant falls. The innovative design of the new bassinet would minimize the risk for such tragic, adverse events by providing a secure and accessible sleeping location for the infant.
Improved access and safety
Promoting mother-infant bonding
Reduced nursing staff burden
The practice of common nursery care is no longer recommended nor facilitated. However, all bassinets in US hospitals are still designed for use by ambulatory nursery staff, rather than for use by mobility-impaired new mothers.

NC State design students assess bassinet needs.
The new hospital bassinets are especially vital for women who deliver by cesarean section, as their mobility restrictions and pain hinder infant care, impede their own recovery, and contribute to risk of infant falls (Tully & Ball, 2014). Cesarean sections currently account for 1.3 million births in the US annually.
The American Academy of Pediatrics (AAP) advocates for new bassinet technology. In 2016, the AAP cited Dr. Tully’s research regarding postnatal unit infant safety in the report “Safe Sleep and Skin-to-Skin Care in the Neonatal Period for Healthy Term Newborns.” The bassinet will be a “game changer” that enables safe rooming-in for infants and reducing undue strain on new mothers.
The promise of Dr. Tully and colleagues’ work developing new bassinet technology for improving maternity care and health outcomes has been described in the leading medical journal JAMA Pediatrics (Wasser, Heinig & Tully, 2017) and reported by The Wall Street Journal (2016).
Request More Information
Bibliography
American Academy of Pediatrics. 2016. Safe sleep and skin-to-skin care in the neonatal period for healthy term newborns. Pediatrics. 138(3), e20161889. [PDF]
Linden, D.W. Increased Division Over Breast-Feeding in Bed.” Wall Street Journal, October 27, 2016. Available at https://www.wsj.com/articles/increased-division-over-breast-feeding-in-bed-1476713700
Taylor, C.E., Tully, K.P., & Ball, H.L. 2016. Night-time on a postnatal ward: experiences of mothers, infants, and staff. In Dykes, F. & Flacking, R. (Eds). Ethnographic Research in Maternal and Child Health. Routledge Press: New York, NC (pp. 117-140).
Tully, K.P. & Ball, H.L. 2012. Postnatal unit bassinet types when rooming-in after cesarean birth: Implications for breastfeeding and infant safety. Journal of Human Lactation, 28, 495-505. [PDF]
Tully, K.P. & Ball, H.L. 2014. Maternal accounts of their breast-feeding intent and early challenges after caesarean childbirth. Midwifery, 30(6), 712-719. [PDF]
Tully, K.P., Ball, H.L., & Ward Platt, M. 2015. The role of postnatal unit bassinets on enabling early breastfeeding. In Smith, P.H. and Labbok, M. (Eds.). It Takes a Village: The Role of the Greater Community in Inspiring and Empowering Women to Breastfeed. Praeclarus Press: Amarillo, TX. (pp. 239-247).
Wasser, H., Heinig, M.J., & Tully, K.P. 2017. The importance of the Baby-Friendly Hospital Initiative. JAMA Pediatrics, 171(3):304-305.
