Antidepressant use in pregnancy may be associated with structural changes in the infant brain
May 19, 2014
A new study by University of North Carolina at Chapel Hill researchers found that children of depressed mothers treated with a group of antidepressants called selective serotonin reuptake inhibitors (SSRIs) during pregnancy were more likely to develop Chiari type 1 malformations than were children of mothers with no history of depression.
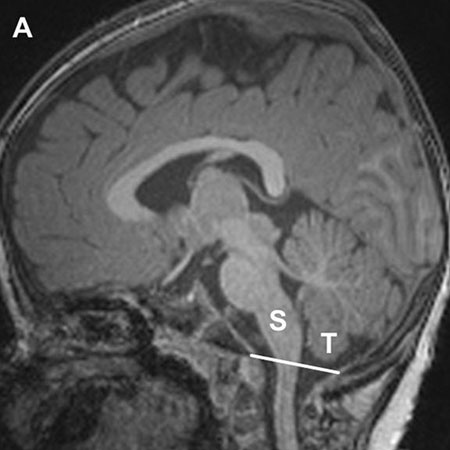
Figure A above shows a magnetic resonance (MR) image from a child without a Chiari type 1 malformation. The cerebellar tonsils (T) are normally near or above the line marking the junction of the skull and spine (White Line). The brain stem (S) has a normal shape.
A Chiari type 1 malformation is a condition in which brain tissue in the cerebellum (a part of the brain that controls balance, motor systems, and some cognitive functions) extends into the spinal canal.
Robert M. Hamer, PhD, research professor of psychiatry in the UNC School of Medicine and of biostatistics in the Gillings School of Global Public Health, is a co-author of the study.
“Our results can be interpreted two ways,” said Rebecca Knickmeyer, PhD, assistant professor of psychiatry in the UNC School of Medicine and lead author of the study, which was published in preview May 19 in the journal Neuropsychopharmacology. “Either SSRIs increase risk for Chiari type 1 malformations, or other factors associated with SSRI treatment during pregnancy, such as severity of depression itself, increase risk. Additional research into the effects of depression during pregnancy, with and without antidepressant treatment is urgently needed.”
The researchers cautioned that doctors treating pregnant women for depression should not change their prescribing practices based on the results of this study.
About 5 percent of children have a Chiari type 1 malformation. Most do not have any problems because of it, but some develop symptoms such as headache and balance problems. In severe cases, surgery may be necessary.
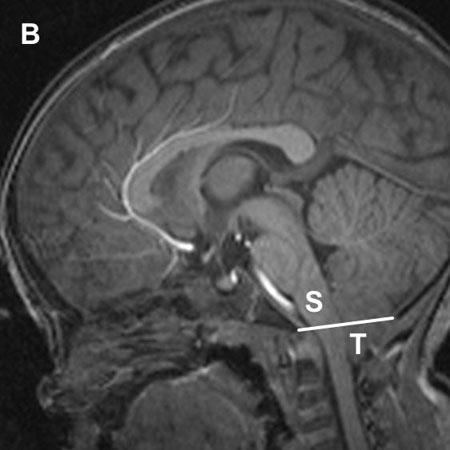
Figure B shows an MR image from a child with a Chiari type I malformation. The cerebellar tonsils (T) are below the line marking the junction of the skull and spine (White Line). The brain stem (S) is squeezed forward and deformed. In some children this can damage some of the important functions of the brain stem, such as swallowing or controlling eye movements. The cerebellar tonsils can also act like a plug, blocking the normal flow of cerebrospinal fluid from inside the skull into the spinal canal. In some children this can lead to fluid build up inside the brain (hydrocephalus) or inside the spinal cord (spinal cord syrinx).
The study’s results are based on an analysis of magnetic resonance imaging (MRI) brain scans done on four groups of children at UNC Hospitals. Thirty-three children whose mothers were diagnosed with depression and took SSRI antidepressant medications, such as sertraline and fluoxetine, were compared to 66 children whose mothers had no history of depression. In addition, 30 children whose mothers were diagnosed with depression but did not take SSRIs were compared to 60 children whose mothers had no history of depression.
Eighteen percent of the children whose mothers took SSRIs during pregnancy had Chiari type 1 malformations, compared to 3 percent among children whose mothers had no history of depression. The rate of Chiari type 1 malformations was highest in children whose mothers reported a family history of depression in addition to treatment with SSRIs during pregnancy, suggesting an important role for genes as well as environment. Duration of SSRI exposure and SSRI exposure at conception also appeared to increase risk.
“These results raise many interesting questions, and there are many things we still don’t know,” said study co-author Samantha Meltzer-Brody, MD, MPH, associate professor of psychiatry in the UNC School of Medicine and director of UNC’s Perinatal Psychiatry Program. “For example, we do not know how many of these children will go on to develop symptoms of Chiari type 1 malformations. What we do know is that untreated depression can be very harmful for women and their babies, and so we strongly encourage pregnant women who are being treated for depression to continue with their treatment.”
Knickmeyer said that a decision to use antidepressants during pregnancy must be based on the balance between risks and benefits and that it is critical that health-care providers and the public receive accurate information on this topic.
She also noted that a diagnosis of Chiari type 1 often is delayed due to the nonspecific nature of the symptoms. Thus, it may be valuable for families in this situation to know about the results of this study.
“Chiari type 1 malformations are somewhat common, but very little is known about what causes them,” said study co-author J. Keith Smith, MD, PhD, professor and vice chair of clinical research in UNC’s Department of Radiology. “Studies like this could give us new insight into that question.”
In addition to Hamer, Knickmeyer, Meltzer-Brody, and Smith, co-authors of the study are Sandra Woolson, MPh; Kenneth Lury, MD; and John H. Gilmore, MD, all faculty members of the UNC School of Medicine.
