Dr. Emily Gower: Preventing blindness from NC to Africa
May 31, 2018
Emily Gower, PhD, is associate professor of epidemiology at the UNC Gillings School of Global Public Health and of ophthalmology in the UNC School of Medicine. Her international research is focused upon improving trichiasis surgery outcomes for people with trachoma, the leading infectious cause of blindness worldwide. In the United States, she researches diabetic retinopathy, which also causes blindness but is 99 percent preventable.
This Q&A with Dr. Gower originally was published on the UNC Institute for Global Health and Infectious Diseases website.
Q. What attracted you to ocular epidemiology?
A. During graduate school, I received a predoctoral training grant from the National Eye Institute. I took a course about the epidemiology of eye disease. Each day was about a different disease, such as glaucoma or cataract. I found the day about trachoma really interesting. We had to develop a study for our final project, and I chose trachoma. The lead instructor approached me after I turned in my project and said she may have some funding for my dissertation based on my idea, and here we are, many years later!
Q. What is trachoma?
A. I work mostly in Ethiopia and Tanzania. Trachoma, which is not common in the United States, is a bacterial infection of the eye. In areas where trachoma is a problem, children can be infected repeatedly. Repeated infection causes scarring of the eyelid. This scarring eventually leads to the eyelid turning inward, causing the eyelashes to rub against the eye in a condition called trichiasis. The lashes cause abrasions on the eye, which ultimately lead to the cornea’s becoming opaque. It is the leading infectious cause of blindness worldwide.
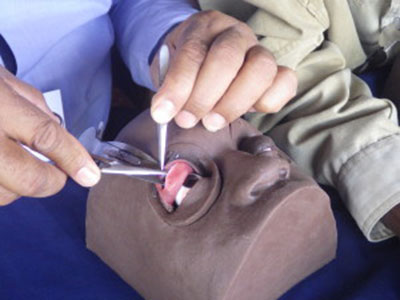
Dr. Gower’s team developed and tested this surgical simulator to bridge the gap between classroom training and surgical practice. Now standard practice in most trachoma-endemic countries, the simulator allows eye surgeons to maintain their skills during the times when no patients need care.
Q. Tell us about your research into trachoma and trichiasis.
A. My research investigates ways to improve surgical outcomes for trichiasis. One problem faced by trachoma-endemic countries is a lack of ophthalmologists. When I started working on trachoma, Tanzania only had eight ophthalmologists in the entire country. The trachoma community developed a surgical training program for lower-skilled workers. These are people with a high school diploma and one year of nursing school. Traditional trichiasis surgery training typically includes a weeklong class, followed by a few weeks of surgical practice. When I started working on trichiasis, surgical outcomes were typically poor, with up to 40 percent to 50 percent of people needing repeat surgery due to poor outcomes. The bulk of my research has focused on trying to make those outcomes better.
My team developed and tested a surgical simulator to bridge the gap between classroom training and surgical practice. The simulator is now standard practice in most trachoma-endemic countries. My team is also looking at other ways to improve surgical outcomes by modifying the procedure and increasing the frequency and quality of supervision.
Q. Describe your domestic research.
A. My research in the United States focuses on diabetic retinopathy and other common ocular conditions. Diabetic retinopathy occurs when blood vessels in the back of the eye become weak and leak. This causes swelling of the retina, and eventually, blindness.
However, 99 percent of blindness from diabetic retinopathy is preventable, and that is why education is so important. We conducted a focus group of people living with diabetes and found that many did not understand the retina’s role in their eyesight and that diabetes can have an impact on the retina. Someone with diabetic retinopathy can have no symptoms or mild vision problems, so they do not realize that something serious is going on.
Educating them about the importance of maintaining their blood sugar levels and having regular eye screenings can help prevent diabetic retinopathy. My research focuses on how to get people living with diabetes into treatment, given that fewer than 50 percent of people with diabetes have regular eye screenings. We are currently exploring installing [ophthalmologic] cameras in pharmacies where patients go to fill their diabetes medication prescriptions. If they get their eyes screened there, they can then get help accessing eye care.
Q. What do you enjoy the most about your job?
A. I am an oddity in the [Gillings School’s] Department of Epidemiology, as there are not many ocular epidemiologists. I have a global health side to my research, too. I have to say that going to Africa and seeing the patients who have benefited from the trichiasis surgery is the most rewarding part of my job. One day, you can see 50 people waiting for surgery who are in pain. Two weeks later, you visit with them and they are happy, and their quality of life has improved greatly. These are people who sometimes walk 10 miles to get to the local market. Not being able to see really impacts their entire life.
Q. What other research questions would you like to answer?
A. Ninety percent of trichiasis affects the upper eyelid, but in 10 percent of cases, the bottom lid also is affected. Current approaches to treating lower eyelid disease are ineffective. I am working to obtain funding to test a new surgical procedure with colleagues at Johns Hopkins to address this. Our initial findings are quite promising!
We also are exploring ways for eye surgeons in these resource-limited settings to maintain their surgical skills between patients and as the number of trichiasis patients is reduced. We are interested in testing whether our surgical simulator can help to maintain skills in areas where there are fewer patients, so surgeons are ready to operate when a patient arrives.
Gillings School of Global Public Health contact: sphcomm@listserv.unc.edu

