Lancet report charts path toward health for sub-Saharan countries
September 26, 2017
A new report on the future of health in sub-Saharan Africa praises advances in certain areas, including maternal and child health and control of infectious diseases, but makes clear that many obstacles – e.g., wars, environmental degradation, lack of resources and others – remain as challenges to the health of these African peoples.
The comprehensive study, published online Sept. 13 in The Lancet, was led by alumna Irene Akua Agyepong, DrPH, who received her doctorate in health policy and management at the UNC Gillings School of Global Public Health in 2000.
Now with the Ghana Health Service, in Acra, Ghana, Agyepong conducted the research with co-authors from the London School of Tropical Medicine and the University of Washington, FHI 360, in Durham, N.C., and from numerous African countries, including Uganda, Rwanda, Senegal, The Gambia, Kenya, Ethiopia and others.
The research was a response to The Lancet Commission – for “The Path to Longer and Healthier Lives for all Africans by 2030.” Established in 2013, the commission has inspired African physicians, scientists and policy makers to chart a roadmap for improved health for sub-Saharan Africans.
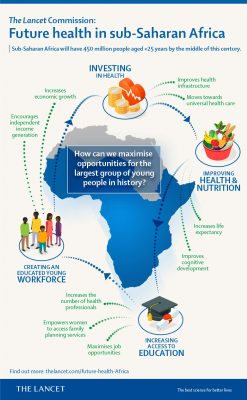
The Lancet Commission highlights 12 strategic options to be considered in African countries’ policies and plans. The options are connected to the health-related Sustainable Development Goals proposed by the United Nations.
The commission highlights 12 strategic options to be considered in African countries’ policies and plans. The options are connected to the health-related Sustainable Development Goals (SDGs) proposed by the United Nations.
The strategies include:
- Control major communicable diseases (HIV, tuberculosis, malaria, neglected infectious diseases and measles), including eradication of polio and dracunculiasis (Guinea-worm disease), and elimination of onchocerciasis (“river blindness”), leprosy, trachoma (bacterial infection of the eye) and lymphatic filariasis (“elephantiasis,” a painful and profoundly disfiguring disease caused by parasitic worms) – and in some countries, elimination of malaria;
- Prevent the spread and minimize the effect of infectious disease outbreaks;
- By 2030, reduce the global maternal mortality ratio to 70 or lower per 100,000 live births, with no country higher than 140;
- Reduce fertility to replacement level;
- Sustain and accelerate decreases in smoking rates;
- Reduce risk factors for noncommunicable disease and promote mental health and well-being;
- Provide essential treatment for non-communicable diseases;
- Reduce incidence of traffic accidents and interpersonal violence;
- End hunger and eliminate stunting; end protein-energy malnutrition and micronutrient deficiencies;
- Achieve universal access to safe water and basic sanitation; promote handwashing with soap;
- Management and equipment of cities for better health; and
- Mitigation of climate change and environmental degradation.
The authors call for urgent action, noting that “the opportunities ahead cannot be unlocked with more of the same approaches and by keeping the current pace.” Rather, they “advocate for an approach based upon people-centered health systems … adaptable to each country’s specific needs.”
“Leadership on Africa’s health, scientific and development challenges should come from Africans, in close collaboration with the global community,” they write. “A fragmented health agenda … will not succeed in strengthening health service delivery and public health systems – and will not address the determinants of health.”
Africa’s young people will be key, the writers say, “to bringing about the transformative changes required to rapidly accelerate the efforts needed to improve health and health equity across sub-Saharan Africa.”
Gillings School of Global Public Health contact: David Pesci, director of communications, (919) 962-2600 or dpesci@unc.edu

